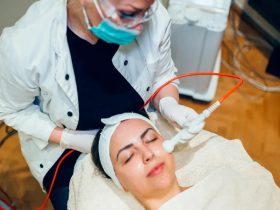
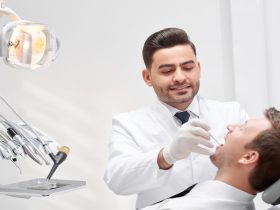
In the healthcare industry, the process of revealing patient-protected health information (PHI) to approved people or organisations is known as the “release of information” (ROI). This well-managed procedure is essential for protecting patient confidentiality and guaranteeing that pertinent medical records are available to those legally entitled to receive them.
It is imperative to have a systematic ROI approach for multiple reasons. It guarantees adherence to privacy laws and rules, safeguards patient confidentiality, and promotes patient-provider confidence. Furthermore, research projects, legal needs, and continuity of care are all supported by an effective ROI process.
ROI solutions encompass multiple stages, each essential to protecting patient data and enabling lawful requests for health information. These stages cover a variety of checks, verifications, and documentation and span from the start of the request to the actual information release.
Phase 1: Request Initiation
Medical information requests can be sent electronically or on paper in various ways. Adopting electronic techniques is consistent with the more significant healthcare digitisation trends.
Securing the request’s authenticity requires robust identity verification procedures. This entails verifying the identification of the person or organisation making the request and their authorisation to access the data.
Legal and ethical issues are brought to light when healthcare professionals start ROI. The need to communicate information for the patient’s benefit, legal requirements, and patient privacy must all be carefully balanced by providers.
When there is a justifiable need for information, typically concerning referrals, coordinated care, or follow-up therapy, providers start ROI. Information dissemination needs are assessed in light of ethical and legal requirements.
A decisive start phase ensures that only authorised entities receive the required medical data and lays the groundwork for a safe and legal information release.
Phase 2: Document Retrieval and Review
Accessing Electronic Health Records (EHRs) is essential for effective document retrieval in the modern digital era. EHR system integration expedites the procedure and allows medical professionals to quickly locate and obtain the needed medical records.
In the case of organisations that still maintain paper records, this stage entails carefully retrieving paper records. Even though it takes longer by nature than computerised techniques, it is still an essential step in the process because it guarantees that all patient data is recorded.
Ensuring quality is crucial throughout this stage. Healthcare professionals carefully check retrieved documents to ensure they are accurate and comprehensive and reduce the possibility of mistakes or omissions.
There are privacy compliance checks before proceeding to the next stage. This entails verifying that the retrieved papers comply with privacy laws and that any possible red flags are swiftly resolved.
Phase 3: Data Extraction and Redaction
When extracting data, accuracy is crucial. Following the idea of giving pertinent information while protecting irrelevant or private information, providers make sure that only the information that is specifically requested is disclosed.
Complete documentation of the retrieved data makes what information has been given evident. Not only is this paperwork necessary for internal records, but it also acts as a guide for future audits and compliance checks.
Redaction is carefully deleting or hiding private information irrelevant to the request. Adhering to healthcare privacy rules and safeguarding patient privacy necessitate this crucial step.
Redaction must prioritise compliance with legislation about health information. It is incumbent upon providers to guarantee that the papers they disclose are compliant with the legislative frameworks that oversee patient privacy and security.
These steps highlight the care that must be taken to ensure accuracy, privacy, and compliance with healthcare standards when retrieving, reviewing, and preparing patient information.
Phase 4: Authorization Verification
A thorough cross-checking of authorisation details is part of this process. Healthcare providers are required to verify the authenticity of the authorisation that has been supplied, making sure that it complies with legal requirements and authorises the appropriate disclosure of information.
Adherence to legal mandates cannot be compromised. Providers carefully check that the authorisation complies with all applicable laws to minimise the legal consequences of unapproved data disclosure.
Clear lines of communication with the person making the request are essential. To guarantee a seamless and open procedure, providers interact with the requester, responding to any questions or concerns and offering the required explanations.
It’s critical to communicate on time. Healthcare providers keep effective lines of communication open, updating all parties on developments and quickly resolving problems to avoid delays.
Phase 5: Release and Delivery
Authorised information is released in the predetermined format, including secure electronic transmission or conventional paper form, based on the requester’s wishes.
During the release, security is given priority. Providers use secure information transfer techniques to protect patient data while it is being transferred from the healthcare facility to the organisation making the request.
Providers ensure that the information they distribute finds its intended audience. This entails confirming the recipient’s identification and following any particular delivery guidelines.
Information releases are recorded to keep an accurate record. This documentation provides proof of conformity with internal policies and laws, which is helpful for legal and compliance purposes.
Phase 6: Documentation and Reporting
As the information release process ends, careful record-keeping becomes essential. Healthcare providers keep an extensive record that includes all information supplied and pertinent particulars, including the requester, date, and reason. This thorough log is an essential tool for monitoring the disclosure history of data.
Providers save information released for later use in addition to urgent demands. By archiving data, you can ensure it’s always available for future compliance checks, audits, or any other type of retrospective inquiry.
Periodic audits are carried out to maintain a high quality of compliance. These audits closely examine the information release procedure to ensure it complies with accepted practices, regulatory regulations, and industry standards. During audits, any disparities or potential improvement areas are quickly addressed.
Reporting is necessary for external openness as well as internal progress. Information release operations are summarised in comprehensive reports that providers produce. Metrics, including response times, the kinds of information released, and compliance with authorisation criteria, may be included in these reports. This information helps procedures be improved internally, and it can be shared externally with pertinent parties to promote accountability and openness.
Conclusion
The process of releasing information involves a systematic journey through several stages. Every stage of the process—from the start of the request to the recording and reporting—is essential to guaranteeing data disclosures’ timeliness, accuracy, and legality.
Three key components are necessary for the ROI process to be effective: timeliness, accuracy, and compliance. Timeliness ensures that the information reaches the requester on time, accuracy ensures that the information given is accurate and pertinent, and compliance ensures conformity to legal and ethical norms.
Healthcare professionals prioritise a culture of continual development because they understand how dynamic the field is. Improved response to changing healthcare demands and increased efficiency are achieved through proactive modifications to the ROI process, regular assessments, and feedback systems.
The release of information procedures continues to be a pillar of the changing healthcare environment, balancing the need for information access and the requirements for patient privacy protection and regulatory compliance.